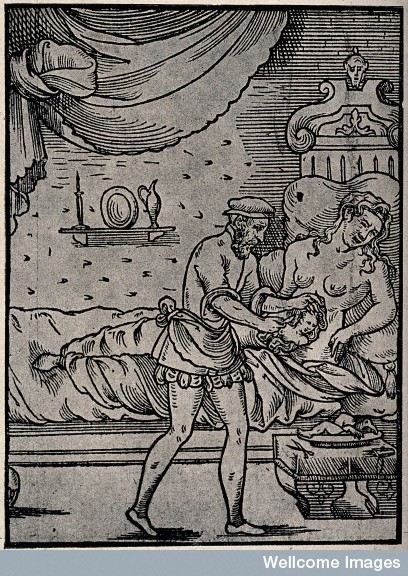
A surgeon performing a Caesarean operation on an agonized woman who had apparently been carrying a dead baby in her womb for five years. Reproduction of a sixteenth-century woodcut, 1933. Credit: Wellcome Images, London.
John Copping, the Dean of Clogher, wrote two letters to Hans Sloane in 1738 about a “Caesarian Operation performed by an ignorant Butcher” (British Library Sloane MS 4055, ff. 293-295, ff. 334-338). Copping first heard about the case of Sarah McKinna of Brentram, which had happened four years previously, from another clergyman. He then visited the McKinna family.
Mrs McKinna married at the age of sixteen. She did not menstruate until after marriage and then it took nearly a decade for her to become pregnant. Two months after giving birth to a second child, Mrs McKinna again developed the usual symptoms of pregnancy. The symptoms continued as expected over the next nine months, but then stopped suddenly. Over the next seven years, she had no menstrual periods and was “perpetually afflicted with the most violent Pains” in her abdomen.
At this point, she developed a swollen abdomen and, once more, the symptoms of pregnancy. Seven months into this “uncertain account”, she developed what she thought was a boil about the size of a goose-egg just above her navel, which gave her “very great Pain” and leaked a “watery humour”. A midwife and three or four physicians visited her, but unable to help, “left her as a dying Woman”.
The “boil” then broke: “from this Orifice started the Elbow of a Child, which hung some Days by the Skin, visible to abundance: At length she cut if off for her own Relief”.* Mrs McKinna sent for local butcher, Turlog O’Neill. By the time he arrived, Mrs McKinna was in “an expiring condition” and “begged him to help her”. He did not do this lightly: “the Man was frightened, and went to sleep”. When he awoke, he acted decisively, giving “her a large Draught of Sack, and I suppose, took one himself”.
O’Neill “made so large an Incision above and below the Navel, as enabled him, by fixing his Fingers under the Jaw of the Foetus, to extract it”. The hole was, according to Mr McKinna, “as large as his Hat”. O’Neill had to pull the bone “backward and forward to loosen it”. Bad enough. But keep in mind,Mrs McKinna was conscious the entire time, her senses numbed only by the large glass of fortified wine.
After removing the jaw, O’Neill spotted something black inside the hole—other bones. He removed as many as he could, but some remained inside, over time working their way out through the navel or “from the Womb the natural Way”. Each instance caused Mrs McKinna great pain.
According to the story that Copping first heard, Mrs McKinna fully recovered within six weeks and only had a small rupture in the belly. The situation was not nearly so cheery, Copping discovered:“She might be about the House, but she was 15 Months confined to the House”. The hole was still so large that Copping was able to “put a Finger a pretty Way up into the Body”… four years after the operation.
Copping, who had sympathetically described Mrs McKinna’s pain throughout his account, raised a collection so that she could be treated in Dublin.
A horrifying case, but it does tell us much about the eighteenth-century world. While we tend to see the experience of pregnancy as self-evident, it was not always so clear-cut for early modern women. Stopped menstruation was not unusual for women in poor health or who lived in poverty, as Mrs McKinna did. Copping, for example, described the McKinnas as ignorant, with poor speech. Mrs McKinna may have had many of the signs of pregnancy, but such signs could also be interpreted as health problems such as dropsy, especially if no baby appeared. In any case, she had a prior history of irregular menstruation.
Copping’s account highlights the growing demands for better medical and scientific evidence during the eighteenth century. He did not just provide the clergyman’s anecdote as fact, but followed it up with the McKinna family in person. He corrected the clergyman’s version: the woman took nearly ten years, not two, to conceive; the woman did not recover as well as rumour suggested; the operation did not occur all at once, but in several parts. By the 1730s just being interesting was not enough for a case to appear in the Philosophical Transactions.+
Mrs McKinna and her “putrefied” baby were certainly medical curiosities at the time. Copping, like everyone else, treated them as such. He noted, for example, that he could not send any of the bones to Sloane because other physicians had already taken them. But he did at least act ensure that the long-suffering woman would receive treatment– unlike the vultures who had scavenged bits of the skeleton without even stopping to close up Mrs McKinna’s wounds.
*Fetuses occasionally develop outside the uterus. See here for a recent case.
+Admittedly, the issue in which it appeared had its fair share of odd cases, from monstrous births to odd items in urine.









